What should you expect?
The National Institute for Health and Care Excellence (NICE)
NICE provides guidance on:
- How different conditions should be treated
- What treatments should be made available.
Learn more about NICE and what they do by visiting their website.
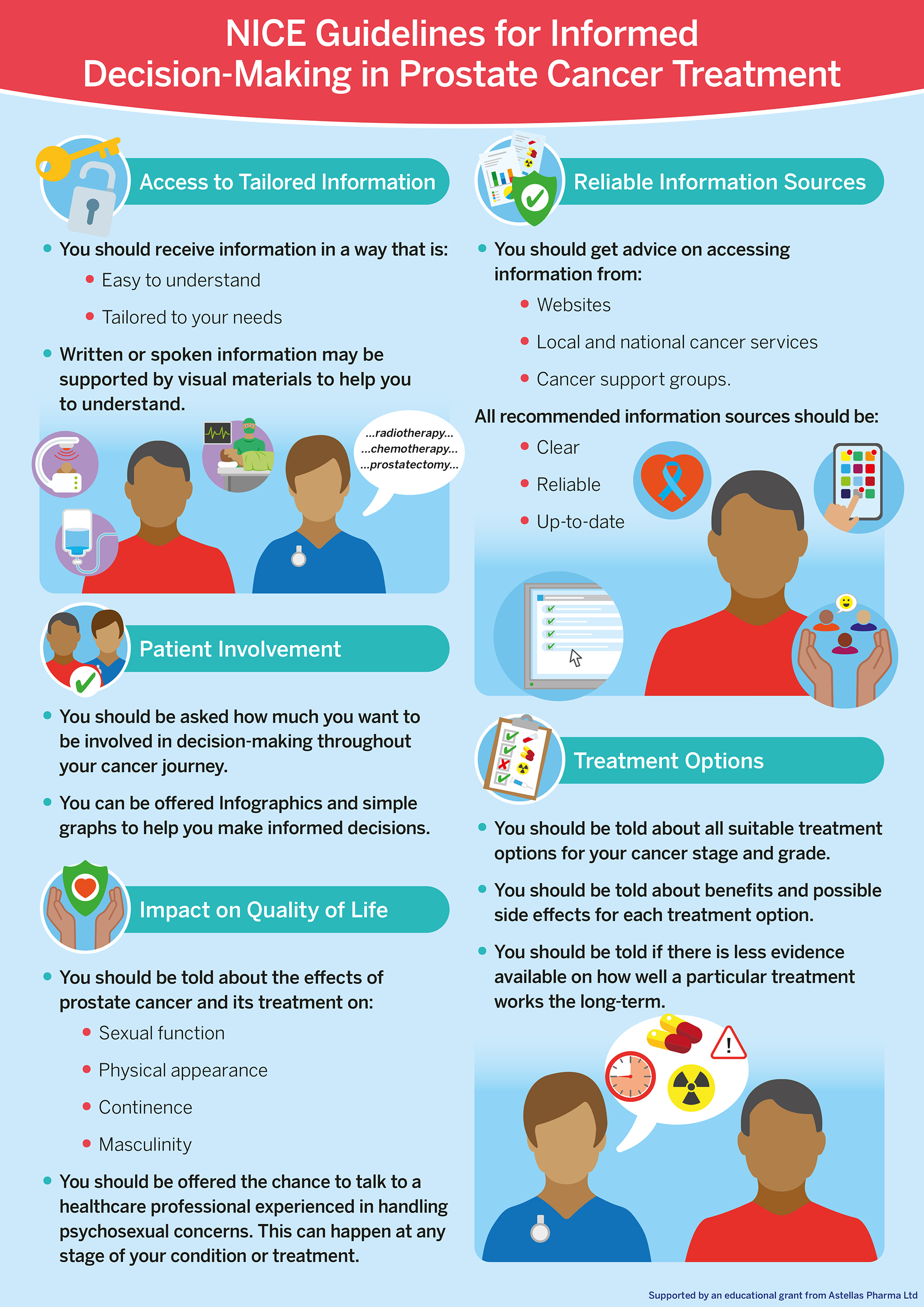
The infographic below outlines what NICE say about what you should expect around informed decision making in prostate cancer treatment. Please note that these are just guidelines and are not a legal requirement. They can help you to start a conversation with your healthcare team about shared decison making.
Making informed choices about your treatment - Tony's top tips
This short animation tells the story of Tony, who has recently been diagnosed with prostate cancer. It starts from Tony's first visit to his consultant all the way through to his final treatment decision. Along the way, Tony gives some valuable tips to help you make a decision about your treatment.
A patient's experience of shared decison making
Listen to Frank, who has been treated for prostate cancer, talk to Colin from NHS England, about his experience of shared decision making.
- Frank also talks about his experience of being involved with a clinical trial called the STAMINA trial (Supported Exercise Training for Men with Prostate Cancer on Androgen Deprivation Therapy). This trial is now closed.
- Visit our page on clinical trials to learn more about this topic.
- Use our clinical trial finder to look for a trial that is suitable for you.
Gathering information to help you decide on a treatment
Before deciding on a treatment, it’s important to learn more about:
- Prostate cancer
- Your treatment options.
Listen to patients Clem, Jack and Jack's partner Laura talk about why they think doing your research is so important.
Can I ask for a second opinion?
- If you want a second opinion, your consultant may be able to refer you to a different specialist within that hospital trust.
- You may have to go back to your GP. This is so that they can make an appointment with a consultant from another trust.
- There is also the option of getting an opinion from a private specialist. If you do decide to take this route, make sure you do your research and look for recommendations.
- The process of getting a second opinion may take time. This may delay your treatment. It is a good idea to discuss with your healthcare team any implications of delaying your care.
Macmillan Cancer Support have a webpage that tells you more about getting a second opinion.
Maggie’s cancer charity explain the advantages and disadvantages of asking for a second opinion.
Ask 3 questions
‘Ask 3 Questions’ is a campaign from the Health Foundation which aims to help patients become more involved in their treatment and care. It does this by reminding you to think about three simple questions when making decisions about your healthcare:
Question number 1: What are my choices?

- Your healthcare team should talk to you about the best treatment choices for you.
- You can ask them why they have decided on those choices.
- You can also ask to speak to both an oncologist and a urological surgeon. This will make sure you get to hear about surgical and non-surgical options (where appropriate). Visit our mastering healthcare conversations page to watch a video about what healthcare professionals you will meet along your prostate cancer journey.
Question number 2: What is good and bad about each choice?

All of our treatment information pages describe:
- The benefits of the treatment
- The risks of the treatment
- The possible impact the treatment may have on your everyday life.
- We asked real visitors to the infopool to share their experience of their treatment.
- They told us how this treatment had impacted their everyday lives in a number of different areas.
- The numbers and images in the impact tab of each treatment page represent how many people said this treatment had impacted them 'a lot' in each of the different areas.
Visit our Explore Treatments page to find out more about each treatment type.
Question number 3: How do I get support to help me make a decision that is right for me?

- Our infopool Explore Treatments tool allows you to explore treatment types or use the "compare" buttons to view methods side by side.
- Our infopool Understanding Treatment Choices tool. This treatment tool aims to help you do four things:
- Understand your possible treatment choices
- Compare these treatments
- Find out more about any treatment
- Discover what might happen if the cancer keeps growing after treatment.
Watch the Ask Three Questions video from the Health Foundation to learn more. The link will open in a new tab.
You can also visit our page called 'Mastering Healthcare Conversations'. This page will give you tips and tricks that will help you have productive conversations with your healthcare team.
Ask 3 questions is part of the NHS's National Shared Decision Making programme. To find out more visit the AQuA website. The Advancing Quality Alliance (AQuA) is an NHS health and care quality improvement organisation in the north-west of England.
About this information
- This information was published in July 2024. Date of next review: July 2026.
- References and bibliography available on request.
- If you want to reproduce this content, please see our Reproducing Our Content page (this link will open in a new external tab).
The toolkit is an information resource for people affected by prostate cancer. The development has been funded through an educational grant from Astellas Pharma Ltd.